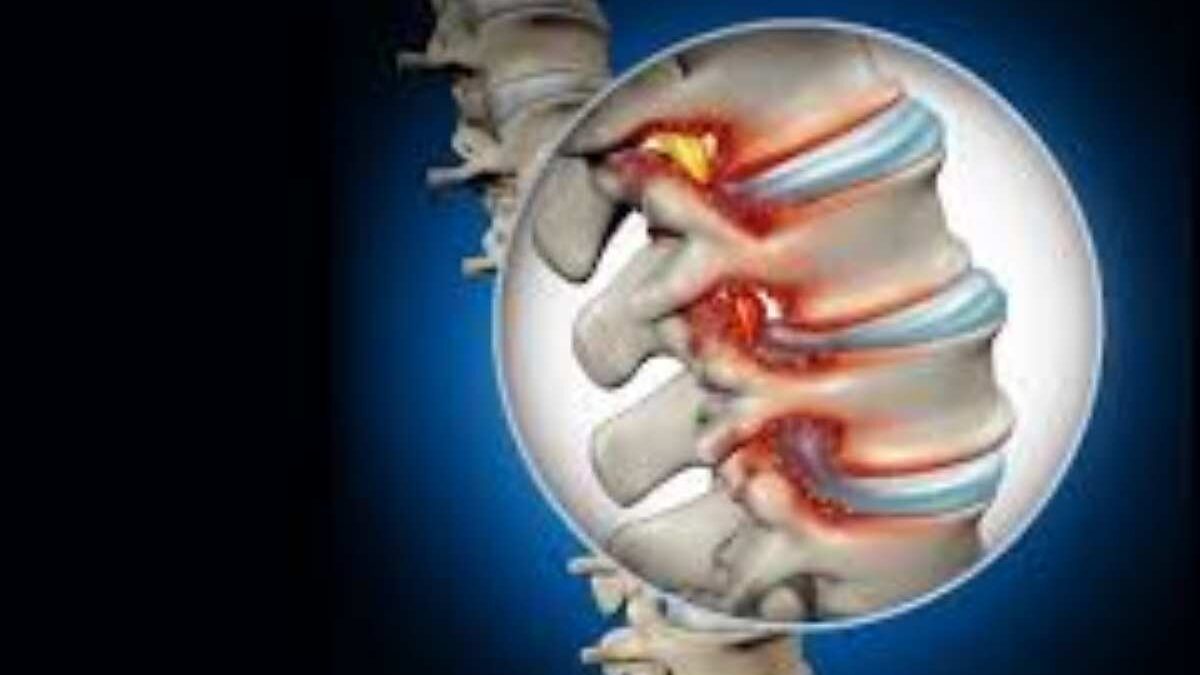
What treatments are available for spinal stenosis? Spinal stenosis is the constriction of the gaps within your backbone. That spinal cord constriction may impinge on the spinal cord or on the branches that lead to pain, numbness, weakness, or difficulty walking – usually more painful when one is standing or walking and less painful when sitting or bending forward. This is mostly localized on the back of the lower part of the body (lumbar stenosis) or the neck (cervical stenosis).
Table of Contents
How doctors decide which treatments to try
The treatment relies on three factors, more or less in the following sequence:
- Symptom severity- mild, annoying, or disabling.
- Impact of the symptoms on your life, do you ever experience any problems walking, sleeping, working, playing?
- Etiology- etiology of the narrowing – e.g., ligament thickening, bone spurs, bulging discs, or a combination.
The majority of clinical practitioners have advised a phase of non-surgical (conservative) treatment initially to individuals who do not have severe or rapidly worsening weakness or indications of spinal cord compression. Operational procedures can be thought of in case conservative treatment fails following a fair trial (typically 812 weeks), or in case of progressive loss of the nervous system.
What is spinal stenosis?
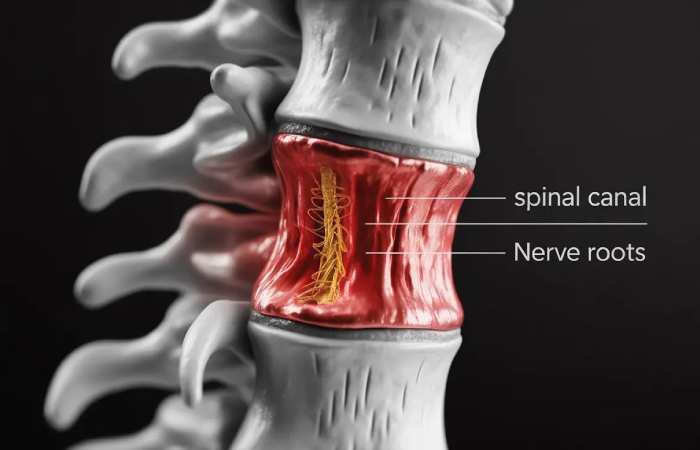
The spinal canal is located in the midpoint of the spine and comprises the nerve root and spinal cord. And it becomes narrower when compressing these structures. This condition is identified as spinal stenosis.
This causes symptoms such as pain, weakness, and coldness, which may differ depending on which area of the person’s spine density is affected.
A person can have either congenital or acquired spinal stenosis. Congenital spinal stenosis means the person has the condition from birth. Only 9%Trusted Sources of spinal stenosis cases are genetic. Acquire spinal stenosis, which is more common and occurs typically after the age of 50 years. Trusted Source is also due to trauma or progressive change.
Acquire Spinal Stenosis causes spinal stenosis.
AS is one of the conditions that can increase a person’s risk of emerging spinal stenosis. And can also damage and wear away bone in the spine. As the body replaces this bone, it creates too much, instigating joints to rage and possibly causing a narrow spinal canal.
Symptoms of Spinal Stenosis
The symptoms of spinal stenosis contain
- Neck pain
- Backbone pain
- Numbness in the arms or legs
- Weakness in the arms or legs
- Hampering
- pain increasing in the leg
- Problems with feet
If a person suffers from pain due to spinal stenosis, this pain may get worse when they walk up and down ramps or steps. You can also relieve the pain by sitting down or leaning over.
People who experience more severe spinal stenosis have problems with the following.
- Bowel
- Bladder
- Sexual
If a person has no symptoms of spinal stenosis, it does not require any medical attention.
Symptoms
Spinal stenosis often causes no symptoms; it starts slowly and does not get as good as the over-dependent part of the spine it affects.
SS Pain in Lower back
This causes lower back pain in or obstructing both legs. This occurs when you stand for a long time or when you walk on.
In the neck
- Spinal stenosis in the neck
- Numbness
- Itchy or weakness in a hand, leg, foot or arm
- Problem with walking and balance
- Neck pain
- Problem with the bowel or bladder
Treatment for spinal stenosis
There are numerous treatment options for spinal stenosis
Surgical treatments — when and what
Surgery aims to create more space for the nerves (decompression) and — if needed — to stabilize the spine (fusion). Surgery is typically considered when:
- symptoms are severe and limit walking or daily life,
- there’s progressive weakness, or
- conservative care and injections have not provided enough relief.
Evidence summary: decompression surgery (for example, laminectomy) improves pain and quality of life in appropriately selected patients. Outcomes are generally better when the correct patients (those with neurogenic claudication and clear radiographic stenosis) are chosen for surgery. Patient.info – Spinal Stenosis (Causes, Symptoms, Treatment)
Common surgical procedures
- Laminectomy / laminotomy (decompression): remove part of the vertebra (lamina) or thickened ligament to make room for nerves. Most common and effective for classic lumbar stenosis.
- Foraminotomy: widens the openings where nerves exit the spine (good when foraminal narrowing is the main issue).
- Spinal fusion: used when decompression could destabilize the spine or when there’s coexisting spondylolisthesis (slippage). Fusion adds stability but lengthens surgery and recovery.
- Minimally invasive decompression / endoscopic decompression: smaller incisions, less muscle damage, shorter hospital stays and often faster recovery for selected cases; not appropriate for all anatomies.
Risks and recovery
- Typical hospital stay varies from same-day to a few days depending on procedure and patient health.
- Risks: infection, bleeding, nerve injury, persistent symptoms, need for reoperation (reoperation rates vary in studies). Recovery includes a graduated return to activity and rehabilitation; many people improve in walking distance and pain within months.
Quick comparison of main treatment options
| Treatment | What it does | Typical candidates | Pros | Cons / recovery |
| Exercise & PT | Strengthens core, improves posture & walking | Most with mild–moderate symptoms | Low risk, long-term benefit if continued | Needs time, motivation |
| Medications | Reduces pain/inflammation | Symptom control for many | Easy to use short-term | Side effects; not curative |
| Epidural steroid injection | Reduces local inflammation & pain | Flare-ups, to enable rehab or delay surgery | Can give quick relief | Short-term benefit for many; not a permanent fix. Procedure risks (infection, bleeding) |
| Radiofrequency ablation | Numbs facet joint nerves | Facet joint pain confirmed by block | Months–years of relief for some | Only treats facet-related pain |
| Open decompression (laminectomy) | Removes pressure on nerves | Moderate–severe cases, neurogenic claudication | Good improvement in walking & pain for selected patients | Surgery risks; recovery weeks–months |
| Minimally invasive / endoscopic decompression | Same goal as laminectomy with smaller incisions | Select patients, centers with expertise | Less tissue damage, shorter stay | Not suitable for all; surgeon-dependent |
Common medication types (role, not dose)
| Medication type | Typical use | Notes |
| Paracetamol (acetaminophen) | Mild pain relief | Generally safe at recommended doses |
| NSAIDs (ibuprofen, naproxen) | Inflammation / pain | Watch stomach/kidney/heart risks |
| Muscle relaxants | Muscle spasm relief | Short-term use advisable |
| Gabapentin / pregabalin | Nerve pain | Can help tingling, burning; side effects include drowsiness |
| Short opioid courses | Severe acute pain flare | Only when other measures fail; risk of dependence |
Choosing between injections and surgery — practical guidance
- Conservative trial (exercise, training, meds) should first be tried in most cases, except in cases of an emergency (e.g., cauda equina signs), or progressive weakness (or other medical crises). There is often a recommendation of structured exercises of a minimum of 8-12 weeks prior to the determination of surgery unless there are emergency questions.
- When conservative care is partially effective but pain flares restrict rehab an epidural steroid injection can be rationalised to achieve a change in inflammation and permit one to continue with an exercise. Try to predict short-term gain; it might not alter the long-term necessity of future surgery in progressive cases.
- In case of a marked impairment in walking, daily functioning, or neurological strength, and imaging corresponds with symptoms, the most reliable opportunity of long-term improvement is likely to be decompression surgery. Address the risk factor, turnaround time and surgical experience.
Rehabilitation and recovery after treatment (surgical or non-surgical)
- Post-injections: persist with an exercise program in order to maximize the short-term alleviation into permanent functional improvements.
- Post-surgery: a lot of them are progressive rehab, which consists of walking, simple moves, followed by strengthening and balance training. The time to recover is different: several weeks in case of minimally invasive procedure, a few months of an open surgery. Until they are diagnosed clear, do not engage in heavy lifting and twisting.
Practical home tips that help right away
- Use a shopping trolley or push a walker for longer walks — leaning forward reduces pressure.
- Plan short, frequent walks rather than long marches; increase distance slowly.
- Practice gentle flexion stretches (as recommended by your therapist). Many people with lumbar stenosis feel better with forward-bending movements.
- Manage weight and cardiovascular fitness — both reduce symptoms and improve surgical outcomes if you choose surgery.
- Keep a symptom diary (what you did, how far you walked, what eased/worsened symptoms) — this helps clinicians tailor treatment.
When to see urgent care or your surgeon ASAP
Seek immediate attention if you get:
- sudden severe bladder/bowel dysfunction,
- new severe weakness in the legs, or
- rapidly worsening numbness around the groin — these could be signs of cauda equina syndrome, a surgical emergency.
Handling of the Spine
The healthcare professional uses their hands to regulate and massage the person’s back, which helps to develop the spine and back muscles.
Acupuncture
This type of balancing therapy entails a physician delivering slender needles to the body at a certain focus area, which is very useful in achieving relief from pain.
Since each of these variants is not applicable, It is vital to inform healthcare professionals about existing ailments so that them to come to sound conclusions in relation to the treatment.
Doctors and psychotherapists can correct the person’s treatment and plan to talk and put up both conditions.
Prevention of spinal stenosis
Therefore, there’s no definite method for people with AS to avoid spinal stenosis. However, by effectively managing AS, a person may be able to reduce extra bone growth in the spine. This, in turn, may decrease the danger of spinal stenosis.
The Arthritis Foundation endorses early and violent treatment for AS to avoid bone damage. A practical action approach will likely include the following.
Medicines
Medicine can reduce irritation and the injury it causes to the bone. This may stop the new bone from rising and prevent several AS problems.
Diet
A food with anti-inflammatory properties can be used to minimize the impact of AS. This diet consists of the avoidance of provocative foods, including the soaked fat and sugar, and the focus on the anti-inflammatory substitutions, including the un saturate fats, fruits and vegetables, and lean protein.
Exercise
This will assist in stiffness and a range of motions, stature, and pliability. Stretching of the muscles and maintaining the muscles can also be accomplished by physical therapy.
Assistive plans:
These devices protect the joint from strain during daily activities. Some examples include supports, splints, and raised spaces to make sitting down relax.
Stopping smoking
Smoking increases irritation and can speed up joint injury. If a person does smoke, they can find help by leaving at smokefree.gov.
Conclusion
Spinal stenosis happens when the spine’s gaps narrow, compression the nerve or spinal cord. Having AS raises the risk of receiving spinal stenosis, as the extra bone that can grow as a result of injury can take up space in the spine.
The signs of spinal stenosis include neck and back pain, impassiveness or weakness in the weapons or legs, cramping, and pain successfully down one leg.